


Ayres, Ian, Sophie Rasman, and Alice Shih. Evidence from Two Large Field Experiments that Peer Comparison Feedback Can Reduce Residential Energy Usage. October. Cambridge, MA, 2009. Cambridge, MA, handy summary is available here. Copyright notice: © 2009 by Ian Ayres, Sophie Rasman, and Alice Shih. All rights reserved.
A few weeks ago, I published my experience at the Health 2.0 Code-a-thon, which involved the development of a rudimentary application that takes medical record data, makes meaningful comparisons to a suitable peer group, and presents it to people, with the goal of stimulating behavior change. The idea for this mash-up came from one of my teammates, who is co-author of this paper (handy summary is available here), Sophie Raseman ( @raseman ), which describes a large scale experiment in using peer comparisons to reduce energy usage. As usual, I see lots of analogies to health care (as did my fellow code-a-thoners a few weeks back).
And what are those analogies? See if you can spot them.
In this experiment, either large numbers of census blocks of households or individual households were randomized to receive a kind of home energy report that contains the following components:
- Comparison to comparable neighbors and “efficient neighbors” with a “normative” (‘here’s where you are’) and “injunctive” assessment message (a smiley or frowney face)
- Twelve-month neighbor comparison
- Personal historical comparison
- Targeted energy efficient advice
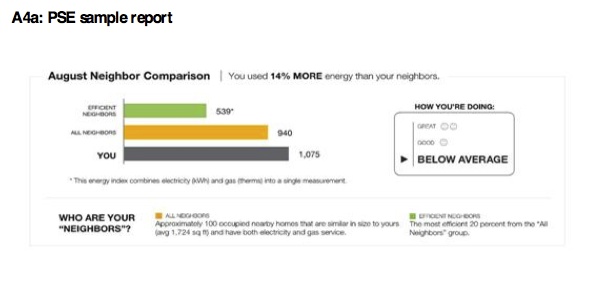

Puget Sound Energy Sample Household Report (click image to enlarge)
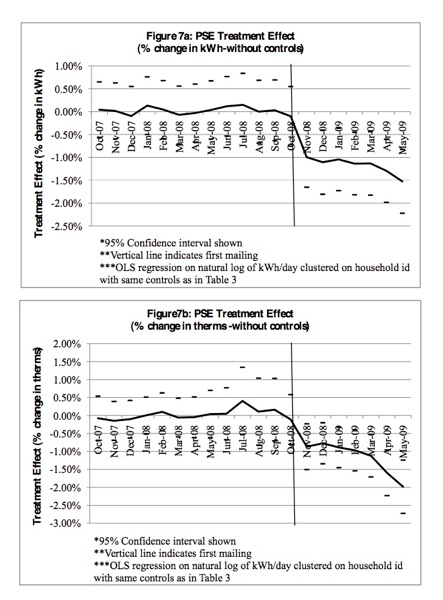
The results: almost immediate reduction in energy use (click image to enlarge)
You can see what an example looks like in the image on the left. They key innovation here, based on studies of social norms messaging by Robert Cialdini and others, is that presentation of relevant peer comparisons with targeted assessments and advice will promote action. And in this case, 85,000 control/intervention homes in the Sacramento Municipal Utility District, and 84,000 control/intervention homes served by Puget Sound Energy in Washington, State, demonstrated action, with 1-2.5 % drops in energy consumption. The environmental impact of a customer-wide program for these utilities would be the equivalent CO2 reduction of 9 and 14.2 million gallons of gas annually.
What’s interesting about this with regard to health and health care is that
- We don’t do these comparisons currently – when was the last time your doctor told you “You are walking less per day than 60% of the patients I am taking care of (frowney face)”?
- There’s an interest in this work in understanding “durable” and “non-durable” behavior. In the study, they measured immediate decreases in energy use from using less on the weekends for example, and potentially more long term gains (“durable”) coming from things like buying more energy efficient appliances.
- There’s understanding of a “boomerang” phenomenon, which is that when people are told that they’re underdoing an undesirable behavior, they tend to feel more comfortable about doing that behavior more. To prevent this, the injunctive message (smiley face – keep up the good work!) is important. Another approach is to not provide feedback to people who are doing well, which also happens to be cost-saving if paper-statements are involved (albeit less appealing in a health care environment where we like to give people good news much more than bad news.)
I had a phone conversation with authors Ian Ayres (who has just published a book: Carrots and Sticks: Unlock the Power of Incentives to Get Things Done![]()
) and Sophie Raseman ( @raseman ) about their thoughts on applicability and there’s enthusiasm for the concepts. They reminded me to focus on behaviors whose change is measurable over a short time horizon – many of the health issues we see have outcomes that take years to manifest.
We also had an interesting (I think) aside about marketing that appeals to people’s interest in rebelling (such as the tobacco industry and a certain computer company that makes phones and tablets), and deconstructed that in those cases, there actually is a component of relevant peer comparisons (because you want to be part of the group that doesn’t use the PC that their parents do).
I think that one of the things that a doctor does is to create a sense of “normalcy” in the patient experience, even in the most health challenged times, to help a patient feel human (“a lot of patients get this, it’s very common” and from this blog post about the history of physician role – “the doctor’s role is to make the patient comparable to himself”).
Maybe what this technique offers us is a way to provide patients quantifiable and meaningful information that appeals to people’s interest in being connected not just to their physician, but to their peers, that piece of the therapeutic relationship that we talk about so much these days. This couldn’t be done very well prior to the advent of health information technology and patient access to their medical information. As a kind of metaphor, this study is based on a much smaller pilot study that involved hand written notes placed on people’s front doors.
The DC-based startup company OPOWER (@OPOWER) has since scaled these techniques in partnership with energy utilities to help shape peak usage in a way that is better for the environment.
So the question is, could these techniques be useful in promoting healthy behaviors? Please post your thoughts in the comments, and if you know of anyone who is using relevant peer comparisons in health care to change behavior, post that information, too.
4 Comments
Ted,
Great post about the parallel worlds – using information to engage consumers and change behavior – that should collide!
I posted about this last fall –
http://www.sharedhealthdata.com/2010/09/12/plug-h…
There's another connection: creating information exchanges (think: grid) that provide consumers with information from multiple sources (say, their electric car, appliances) to gain benefits and reduce costs. I see…connecting to the TV to get your energy consumption, lab tests, appointments….all centered around a person's life. It's not for everyone, but hey, tipping points happen.
As for using comparative data feedback – there's solid evidence about this to change provider and system behavior. Northern New England Cardiovascular Study Group, Maine Medical Assessment Foundation (my former employer), Jack Wennberg and other pioneers in reducing care variation – were the nidus for the Quality & Performance Era. While data is power it's insufficient. How messages are delivered (displayed)…who delivers….how they're "socialized" and marketed….and all the intrinsic and extrinsic motivators that can facilitate change…are critical.
http://www.ncbi.nlm.nih.gov/pubmed/10169780
I think we can learn a LOT about consumers from the energy arena (and others). I think they can learn a lot from healthcare and behavioral science.
RT @ericaholt: Can peer comparisons promote healthier behaviors (a la @OPOWER for energy use)? by @tedeytan http://teyt.in/f2OxoZ
Free Reading !!! Now Reading: The @OPOWER experience – peer comparisons can reduce …: Com… http://bit.ly/dO1Rnt mypsychicsonline.inf
Fantastic post, Ted! As a fan of OPower for some time, intersecting social marketing, social networking and graphic design is where healthcare must go. Boldly.
http://tinyurl.com/98qbrv9
But also for healthcare team members! How about:
90% of providers responded to secure email within 24 hours.
90% of residents ask patients to sign up for online access to their information
🙂