
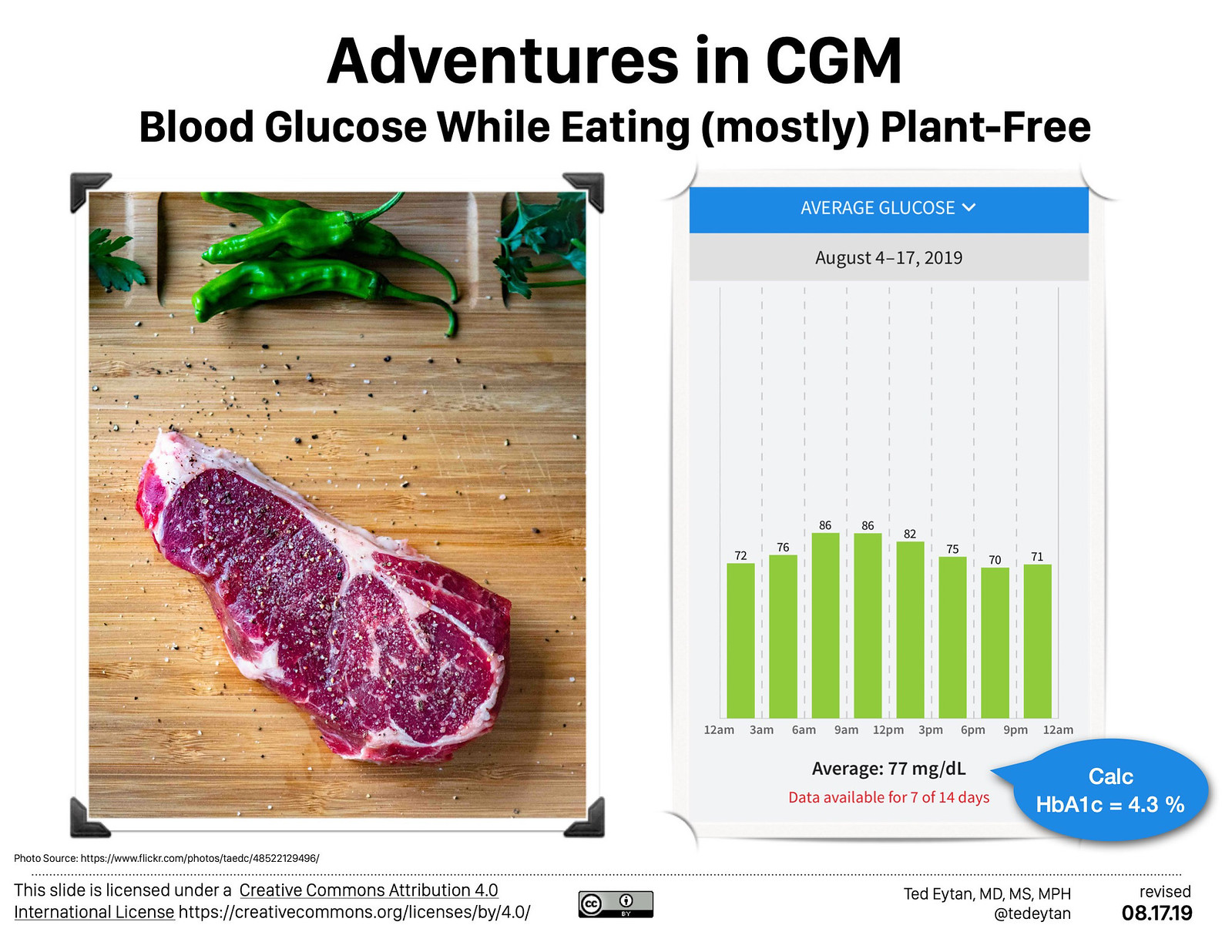
The numbers above and below are continuous glucose monitor measurements while eating a (mostly) meat diet for a few weeks. As the images show (and people seem to forget…), meat includes fish.
As predicted, the numbers are normal, and very stable, given meat’s glycemic index = 0. I would say they are more stable than previous measurement periods. In a person without prediabetes or diabetes, the difference isn’t materially signifcant though.
An average blood glucose of 77 mg/dl calculates to a HbA1c of 4.3 %. Laboratory measured HbA1c’s can be highly variable, based on red blood cell characteristics…
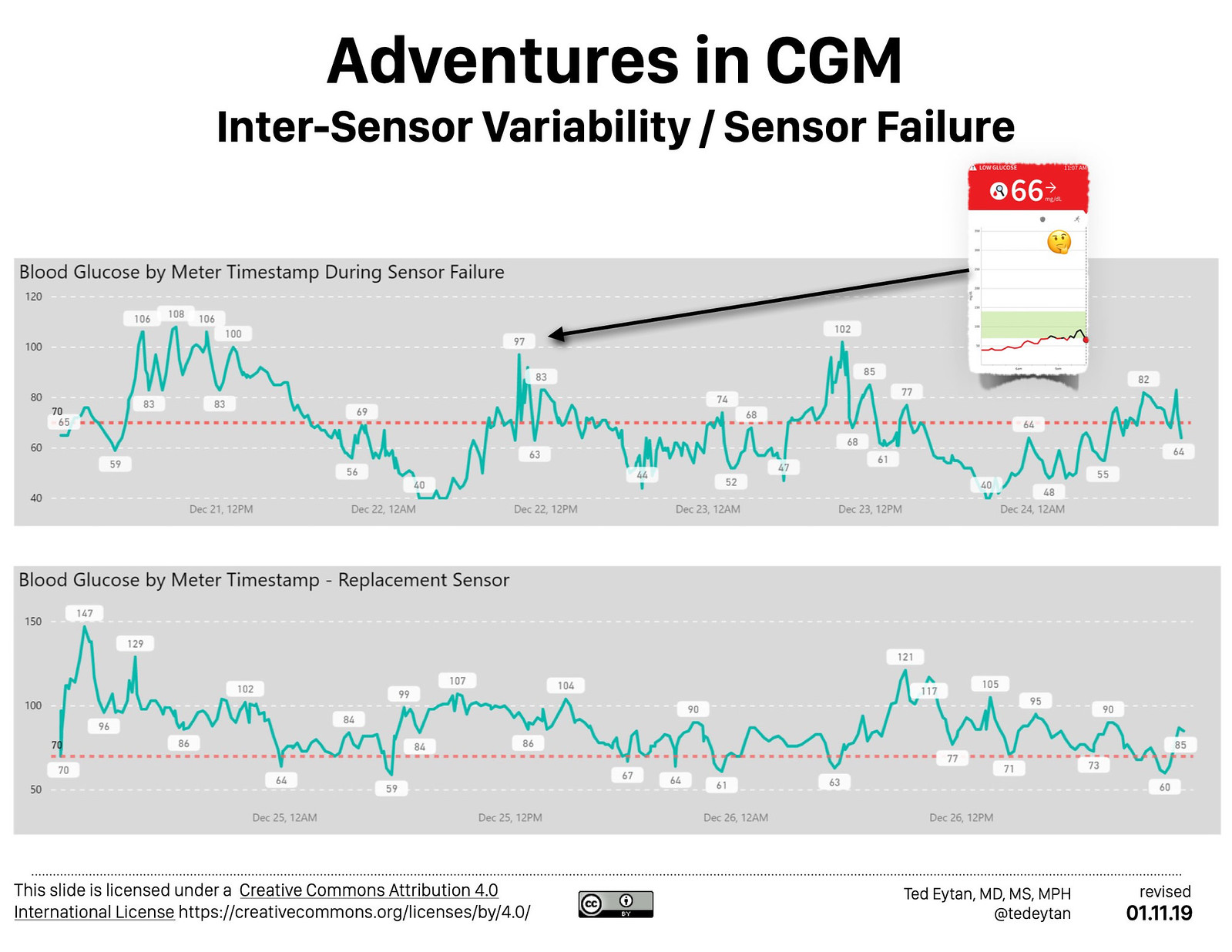
I have also found from my experience that every sensor is slightly different. See below for an example of sensor failure.
What am I getting out of wearing a CGM? Answer: A lot
I have been getting this question (or comment) from people who know or don’t know that I’m a physician. It’s a reasonable one given that most (all) of the readings are within normal levels.
Understanding glucose metabolism for the first time
I’ve discovered from this experience that I never learned how the human body so elegantly metabolizes glucose. I’m not talking about biochemistry and physiology – we learned these in depth. Many of my professional colleagues still don’t know or understand, except through the review of lists of manually obtained glucose readings, some with context, some without.
It’s incredible what the human body can do & to see it in action for such an important metabolite. The converse is also true, it’s important to understand the situation where the body cannot manage this metabolite and how it may struggle for equilibrium.
This type of data is orders of magnitude more important for a population, than say, a 1 lead EKG as certain wearable devices are acquiring 🙂 .
Understanding the life of a person with diabetes
I have had people approach me asking, “Type 1 or Type 2” when they see the sensor. I answer “neither,” and then a great conversation ensues.
In the LGBTQ space, I say people who don’t identify this way will never ever know what it’s like.
For diabetes, I do not know what it’s like, however, it’s possible that I could in my lifetime, depending on my metabolic health status. 88% of Americans are at risk to know what it’s like.

What I hear in ways I haven’t before, and can corroborate from my own experience, is about the way people with chronic illnesses are treated. There’s also a differential in the way type 1 and type 2 diabetes are recognized and respected (or not) in our medical system. We can always do better.
Sensor failure
An experience that stands out in my mind is the phone call I made to the manufacturer when a sensor began to malfunction. The way in which I was interrogated, clearly off of a script, was something bordering on inhuman. Not the fault of the person on the other end of the phone, just a marker of the way our society approaches people with health challenges. Interestingly, once I passed through the gate as it were, replacement was made quickly, efficiently, satisfactorially. What it took to get there I will never forget….
As I have said in other contexts with people working to control their health and life destiny, I wish this experience on every nurse and doctor in their career. It will help them be better for the people we/they serve.
Reminder of my disclosures
I’ve created a page specifically addressing any conflicts (I have none).