
This paper, published in 2017, provides an overview of studies and potential applications of continuous glucose monitoring (CGM) done to date.
The paper is of interest to me as I’ve been wearing a CGM as a non-diabetic, normoglycemic, physician for some time now (see: Part 1: Why I decided to wear a continuous glucose monitor as a non-diabetic physician , I’m now up to 8 parts of this story).
The paper confirms a few things I assumed were true:
- We don’t really know how to use continuous glucose monitoring in medicine yet
- Like all monitoring devices, information does not necessarily lead to improvements (see the saga of activity monitors and their lack of efficacy: Just Read: Listening to Physiology instead of a Wearable for Weight Loss)
- The state of the technology is impressive, but not yet stable or as accurate/accessible as it will be in the future.
Not a single mention of diet
I realize I live in, and am from the future, however, I am still impressed that a comprehensive review of the technology does not mention the role of managing glucose metabolism via diet. Not a single time. If we know that 55% of Californians have insulin resistance now, and these numbers are rising, the potential to prevent or reverse diabetes should be topic of discussion in the use of the technology.
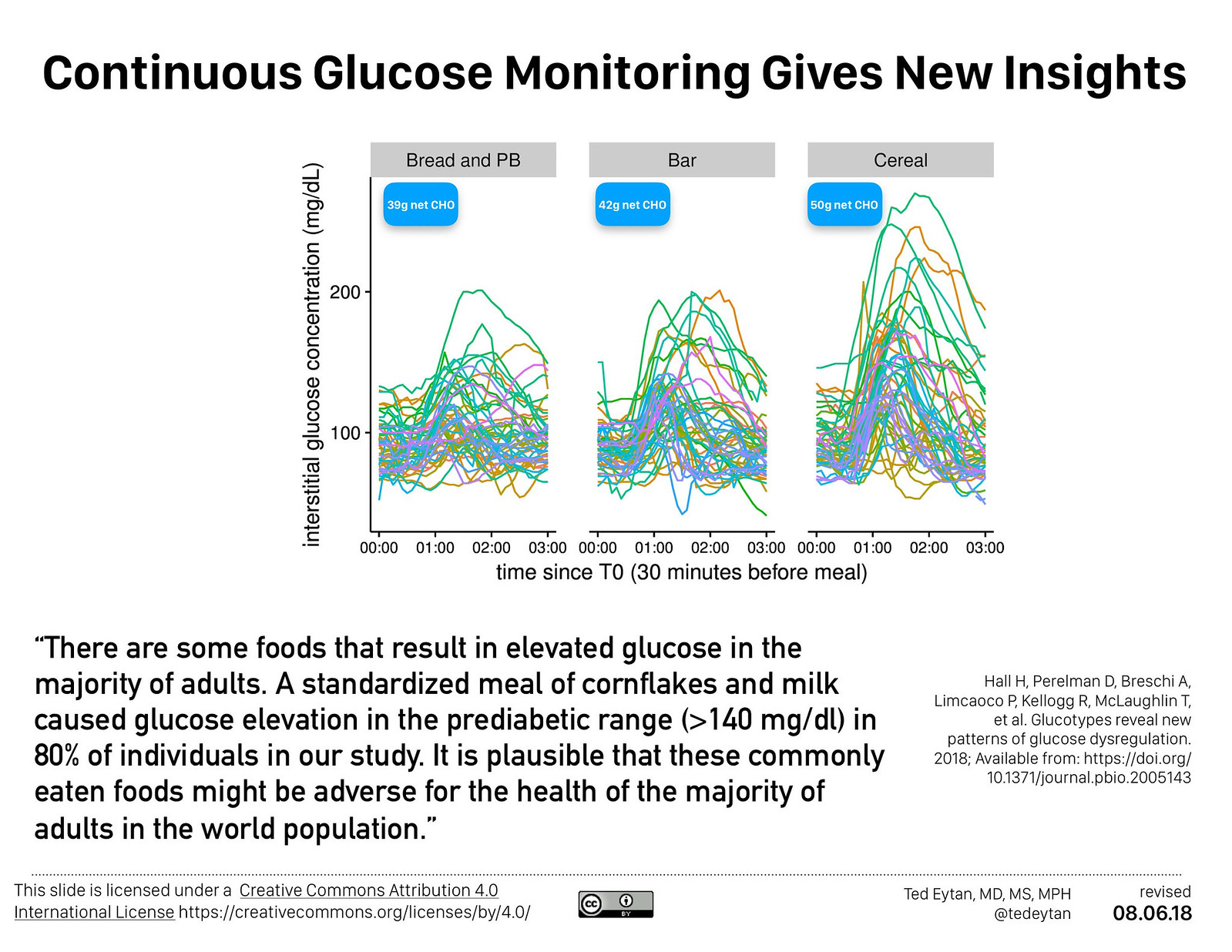
In my own experience, I have been able to document how a CGM, for the first time gives an insight into glucose metabolism, of the kind we have never seen before in our clinical lives. This the pattern I see, eating a low carbohydrate, healthy fat diet:

Note the lack of glucose peaks (“excursions”) compared to a cross section of people eating a variety of “standard diets”, and the one with the worst pattern is the meal that was the lowest fat, lowest calorie.
Reminder, My Disclosures and this is not promotion of CGM for all
I continue to enjoy a conflict-free existence, and I am not promoting CGM for all. Review this post and my disclosures page.