A few spare moments digging into the treasures not hidden within data from the Pew Internet & American Life Project (@pewinternet) plus my own archive tells an interesting story in preparation for Tech Demo Day:
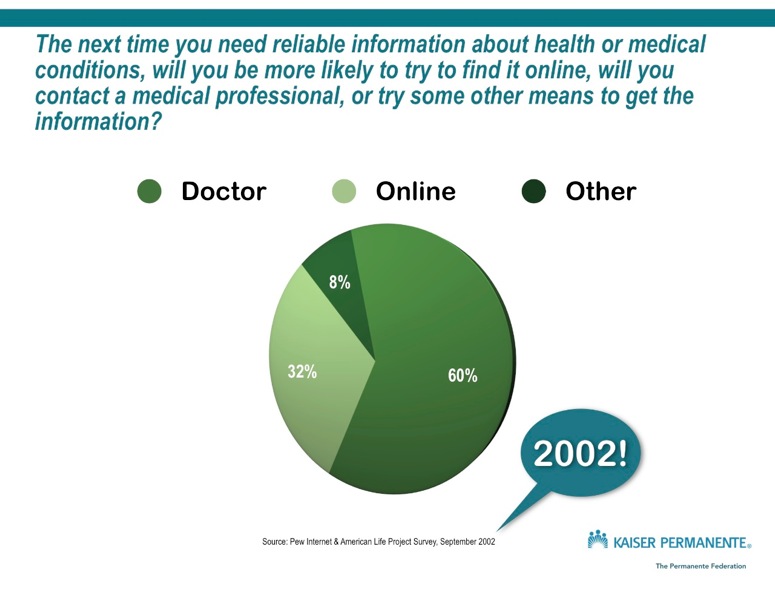
In 2002, it seemed like the physician / health professional role would become obsolete. More people were choosing the online channel to get health information, and the numbers were rising. This is the original slide I used from a deck way back when….
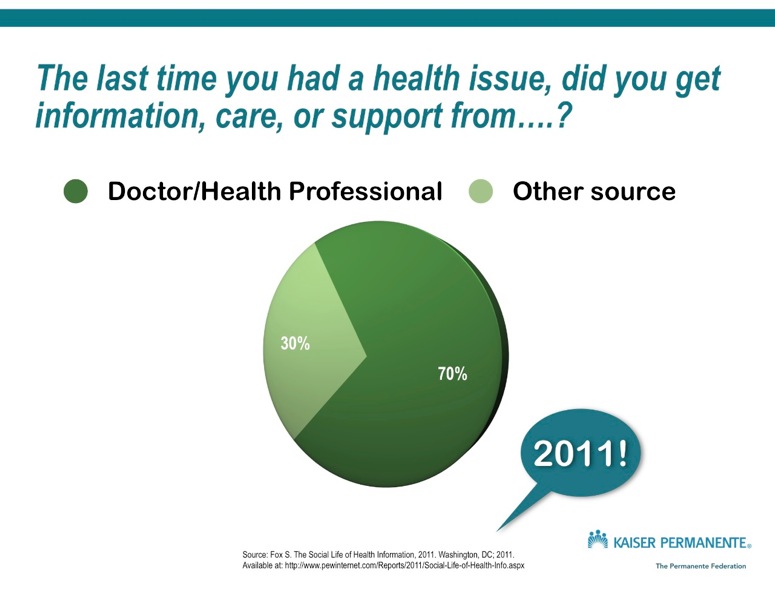
Let’s clean it up with a more modern design before we continue (have to do it…can’t help it) and compare it to data from 2011, note the question is a little different, this time it’s “the last time you had,” versus “the next time you need”
So the doctor/health professional didn’t become obsolete; they are still the #1 most used source for health information, friend and family is #2, internet is #3
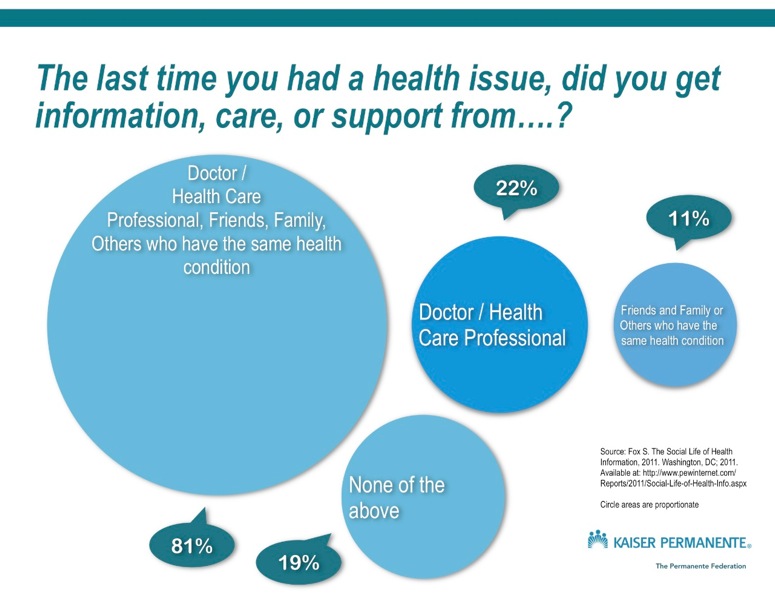
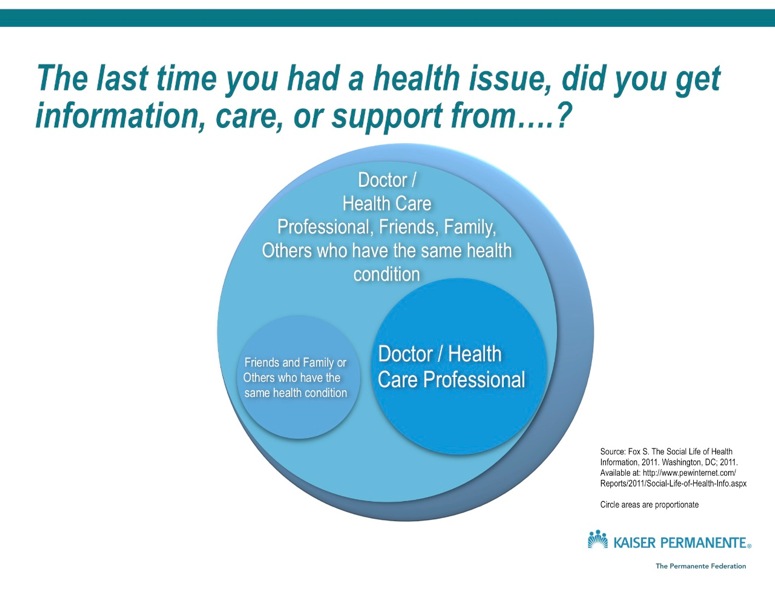
However, the story doesn’t stop there. When I recompiled the data a little (check my work here, @susannahfox), I found that the doctor/health professional is an important part of a whole ecosystem of information and support. So it’s not like the top image on the left – that one seems to imply that each source is mutually exclusive, when it’s not. It’s more like the middle image on the left, whose data shows that 81% of health issue support/information comes from a combo of health professional, friend/family/other person with condition. This actually looks lot like the bottom image on the left, which is the world renown Chronic Care Model, developed way before the internet was famous. The challenge is that these sources of information are not currently well integrated in the health care system.
Enter the friend/family/other side of the equation – “quantitative crowdsourcing“
A few recent posts on CureTogether.com‘s (@curetogether) blog reveals an interesting trend to me as a physician – people tend to self-assort to treatments that are effective and generally less invasive (which translates into more effectiveness, lower cost).
Take a look at the work they have done for Back Pain: Lower Back Pain Study: 2,300 Patients Rate 46 Treatments. As a doctor, there’s one data point that catches my eye – it’s the one for the drug gabapentin (listed as its trade name, Neurontin). It’s not very popular, not very effective with patients. Turns out, it’s not very popular, not very effective for physicians either, after a court ruled that it was illegally marketed for uses other than for what it was intended (epilepsy).
By integrating our worlds a little, we can learn that our patients are smarter than we sometimes think.
Take a look at one more example, Urinary Tract Infection: Antibiotics or Cranberry Juice?. This one is a riff off of an Archives of Internal Medicine study recently published comparing the effectiveness of cranberry capsules to low dose antibiotics to prevent recurrent urinary tract infections. The crowd shows a superior response to the antibiotics, which is what the researchers found. However, there’s another important finding of the researchers – that antibiotic users had large increases of antibiotic-resistant bacteria in their bodies, and to say that one treatment is superior has to factor that in – here’s what they said:
For rational decision making at a societal level, we will perform a cost-utility analysis, weighing effectiveness of prophylaxis against the costs of increasing antibiotic resistance.
Just like it says in the data above – everyone is necessary. It’s worth learning more about, isn’t it?
I would also say it’s worth learning about from people who value patient centered-ness and (in true Generation X from), collaboration over “winning.”
This is why Alex Carmichael (@accarmichael) and Daniel Reda (@Dreda), the founders of CureTogether.com have agreed to come and share at our technology demo day, so that an audience engaging in integrated care delivery could visualize what it might be like to engage in social networking to enhance a care relationship. Exciting!
In true social media form, I use blog posts to audition content and make sure it’s accurate, please check my work, make it better, faster, stronger before the big day.



8 Comments
Wow, thanks Ted, for your interesting, nuanced, and supportive take on our work!! One tiny correction – I’m @accarmichael, with 2 c’s. We are honored and excited to be part of Tech Demo Day. 🙂
Alex,
Thanks for the improvement, it’s fixed, and keep them coming, to this post and to health care in general :),
Ted
Thanks Ted, you are amazing!
RT @tedeytan Why link quantitative crowdsourcing &care delivery : @CureTogether at @KPGarfield Tech Demo Day http://t.co/OfrL8NJ #hcsm
RT @healthythinker @tedeytan Why link quantitative crowdsrcng & delivery @CureTogether @KPGarfield Tech Demo Day http://teyt.in/nZovbg #hcsm
Post: The case for linking quantitative crowdsourcing and care delivery : @CureTogether at @KPGarfield Tech Demo Day http://t.co/OfrL8NJ
RT @tedeytan The case for linking quantitative crowdsourcing and care delivery: @CureTogether at @KPGarfield Tech Demo.. http://t.co/OfrL8NJ
RT @tedeytan The case for linking quantitative crowdsourcing and care delivery : @CureTogether at Tech Demo Day http://hisoc.us/ovRpNE