This is second of a multi-part series on a patient’s experience managing a chronic condition, in this case hypertension. We’re now past the discovery that something may be wrong, and at follow up with a personal physician. Recall that 1/3 of patients do not make it this far.
Click on the image to see it larger size
Patient Story (Frydman)
I was convinced that the HBP was just a temporary event due to stress and that by the time I had it checked by my friend the problem was gone. The measurements showed that I was completely mistaken. For the first time I was faced with the possibility that I was not really in control with a health problem. Even after a couple of measurements and a strong admonition from my friend to take every day the medicines he prescribed, I was still inclined to deny the reality of the problem. I remember telling myself: ” even if the problem is there to stay I can still afford to wait another 6 months before I become a compliant patient.” And I kept being this stupid and stubborn patient for another 1 1/2 year.
He said: “this is very dangerous. We do not want you to experience a catastrophic event. Therefore you must be treated”
For some reason, that is NOT the message that makes me understand that I really must be treated. There is clearly a missing piece in the way the doc is interacting with me, his friend. By spending maybe 3 to 5 minutes explaining the rational behind the proposed treatment he would have transformed the interaction from – he is forcing me to change – to – I understand why I must change
I was supposed to go back but I didn’t do it. During a business trip I did try checking my BP with a home tool a few times and every time the BP was well within the norms, helping me be even more in denial. But then the next time I went to my friend’s office the data still showed clear HBP. Go figure!
Clinical and Public Health pearls (Houston-Miller)
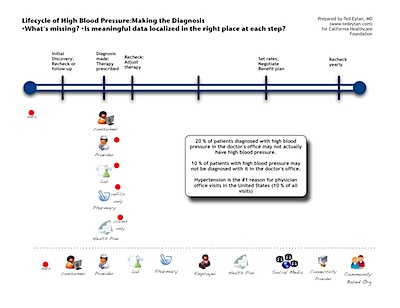
- Hypertension is the #1 reason for physician office visits in the United States (9.7% of all visits)
- 20 % of patients diagnosed with high blood pressure do not actually have it; it is falsely elevated in the doctor’s office (called “white coat hypertension”). This results in unnecessary (and costly) treatment.
- 10 % of patients measured with normal blood pressure in the doctor’s office actually have high blood pressure (called “masked hypertension”)
- In recognition of the above, many health plans and Medicare reimburse for “Ambulatory Blood Pressure Monitoring” (CPT Code: 93784), which is a 24-hour, round-the-clock, blood pressure measurement. This type of measurement is typically a research tool and not used in clinical practice. There is no reimbursement for home monitoring currently.
- The average of 2 home blood pressure readings is more predictive of mortality than screening blood pressures taken by nurses and technicians
- 32 – 53 % of patients stop their medications by the end of the first year
- A patient like this is considered “high risk” because he is male and likely to have another condition (such as high cholesterol)
Comment
Where is the data? The diagram and patient’s experience illustrate the fact that the information related to the diagnosis and treatment is typically localized to the provider, and not the patient. When a diagnosis is made, lab studies and medicines are ordered, and the patient’s health plan will receive a claim for the office visit. The patient is typically instructed to come back to the doctor’s office for reassessment, rather than doing self-assessments, and the patient is usually not given a treatment plan, or access to blood pressure and other data generated in the visit.
What’s missing? As in the previous vignette, the patient is without information regarding the significance of the condition, or resources to learn more / compare with other patients’ experiences. In my own searching, I have found limited social networking resources online for blood pressure management, relative to other conditions such as diabetes. This is beginning to change, though, as more organizations, such as the American Heart Association, become active in promoting self-management and personal health records.
Tomorrow, ongoing management and maintenance of blood pressure control. Comments welcomed, of course.
16 Comments
I'm fascinated with the idea of a Bluetooth-enabled (or WiFi) home blood pressure device, which uploads its data to a mother ship somewhere. Does such a device exist?
Dave,
Not 100% sure about this – I am not familiar with all the device types yet. You could consult the selection available at either Microsoft's HealthVault site or iMetrikus' site to see what's currently available. I anticipate that something along these lines will be available soon, if not already. After all, you can now buy an SD card for your camera that includes a built-in Wi-Fi transmitter to "the cloud." Why not for this,
Ted
Ted, I am one of the EMHA students you practiced your presentation on recently. I am a family doctor in private practice. I appreciate this example you present as characteristic of paternalistic medicine (even when the doctor is a close friend of the patient). However, I hope you appreciate that even outside of Group Health there is a diversity to how blood pressure is handled. In our office (somewhere along the diversity spectrum of BP management) while evaluating the diagnosis with supporting evidence we give the patient background info on the risks of high blood pressure and an expectation of what a normal level is. We look for three high readings before making a diagnosis, usually with some outside the office measurements. Rather than high tech approaches like wifi or bluetooth, we like to use the telephone for connectedness outside the office to check in with the patient on home readings. Someday soon we will have secure messaging available as another channel.
I'm interested to see how your 'mental model' on patient centered managemenet develops.
Hi Mark, Thanks for stopping by! I am actually outside Group Health now, a family doc, living in Washington, DC, so how can I not appreciate diversity at this point :).
It sounds like you have a nice approach to assessing blood pressure. Do you do the three high readings in the office? How do you incorporate home monitoring? Do you give patients a protocol like the AHA recommends (7 days, morning and evening only).
Do you counsel patients on technique in the office? Last question – do you recommend certain types of monitors to patients?
We're looking for best practices, so thanks for taking the time to share what you do for patients, and to comment and critique along the way,
Ted
I'll butt in and say that my wife and I have recently started using the Omron 790IT and we love it. I selected it for its ability to upload to a PC, which I know isn't everyone's cup of tea. But it has an unexpected feature, "TruRead," which will automatically pump itself up three times in a row and display the average.
In practice this saves me from (mindlessly) wondering whether I'd get different results if I ran it again.
Hi Dave,
How often do you check?
And….how did (or didn't) your doctor bring home monitoring into the discussion about your health? Were they encouraging? Did they tell you how to do it? What did they say?
I have one more installment in this series to pen…coming soon,
Ted
We've just started using it (within the past week) so reliable compliance hasn't been proven. 🙂 But in our imagination, it will help us do what we always meant to do – check in the a.m. and p.m. (This Omron machine has a special alert for Morning Hypertension, which it claims to detect by looking at its history. It has settings for user A, B, and Guest.)
I've been checking BP at home for years. Our earlier one was a manual Omron "squeeze the bulb" thing. I frankly don't remember who brought up the idea. Maybe he does – I'll ask if he remembers. (He, like many other MDs, astounds me with his ability to remember things I did years ago.)
Fair warning, though; my guy is Danny Sands, a card-carrying member of the e-Patient Working Group, so he's way ahead of the curve on some things.
Dave,
Yes, please ask him. Did he advise you to monitor (or does he now), did you pick up the idea on your own, and how does he recommend you (or a patient) do it – e.g. how many days, what time of day – is it systematic or is it a general "you should home monitor." How does he want you to deliver that information to him, or does he want to use his own measurement in the office or both?
I'm putting my eggs in the same basket as yours – Danny's going to be Dr. ahead-of-the-curve – but let's change the locus of control toward the patient, one conversation at a time,
Ted
Hi, Ted. e-Patient Dave alerted me to your post and discussion.
I think I asked Dave to monitor at home, as I do with many of my patients. For Dave it's helpful because he lives far from my office, but for most of my patients it's more useful to have additional BP datapoints, rather than just the highly artificial office measurements. It's also quite empowering for patients, but the data must be shared with the care management team so that treatment can be appropriately adjusted. Also, it's important to educate patients about how to use (or not use) this information. Finally, the measurements with the home equipment must be compared in the office so that we don't get misled by incorrectly high or low readings.
In addition (and as I'm sure you're aware), there is a growing literature supporting home BP monitoring in the diagnosis and management of hypertension. Some examples:
Green BB et al. JAMA 2008 Jun 25;299(24):2857-67.
Home monitoring plus pharmacist via secure web communication (but not without pharmacist) improved control vs. usual care.
McManus RJ. BMJ 2005 Sep 3;331(7515):493. Epub 2005 Aug 22.
Patient self-monitoring (although in the office) resulted in just as good care as doctor visits.
Stergiou GS, Kalogeropoulos PG, Baibas NM. Blood Press Monit. 2007 Dec;12(6):391-2.
Review article. Home monitoring has excellent prognostic value and is even better than office measurements.
Also, both the US and Canadian BP task forces recognize the value of home BP monitoring.
Best regards.
– Danny
Thanks for stopping in, Danny!
So the detailed question is, do you follow a protocol, as recommended by the AHA position statement – 7 days of readings, once in the morning, once in the evening, not done during the day, averaged, and repeated every quarter? Or is it a more generalized support for home monitoring?
What I've been finding is that recognizing the value and making it standard of care are two different things. Our walkthrough with the patient and the clinical experts showed that at the end of the day we still default to the doctor as locus of control.
The Green study was nifty wasn't it – it was performed at Group Health during my tenure :).
Thanks for taking great care of Dave and e-patients everywhere,
Ted
VOP here. (Voice of the Patient, analogous to VOC:
Not that anyone asked, but: "protocol schmotocol." All I know is, he recommended I do something (probably) and I did what I did, which vaguely remembered his recommendation.
I don't mean to be glib or punky, but that's reality, and you can quote me.
One of my current explorations is: what's the difference between how people are about oil changes (in their cars) and routine maintenance of their carcasses?
I know that's not deeply philosophical (much less metaphysical) but that's what you get tonight.
Truth is, I went through seeing a few cars not do so well when I neglected routine maintenance, and have decided that long term it *is* worth the effort to take care of things. Hence the recent purchase of the upgraded Omron.
I think this industry will be a lot more effective once everyone realizes how well PC users observe methodical backup practices. (i.e., not very much.) What do we do THEN?
Okay, back to you guys.
(How come your blog doesn't have Preview for comments?)
Dave,
The VOP is always prioritized here. Should we just adopt the VOC definition – or do we start another crowdsource for that one :).
I understand a protocol doesn't mean much to you – that's helpful. The reality that I/we see is that in the absence of a guideline, there is a slient one – doctor in control. If a new protocol for managing an illness (directed at clinicians) isn't the answer, what is? This is what AHA proposed in May…
I will take your thoughts under consideration as I post the next installment in this series. I'm glad you're engaged – this blogging thing works,
Ted
Ted, sorry I didn't get back earlier. I know you are not at Group Health now, but figured that was your last clinical experience.
I do not require three readings in the office for diagnosis, but I aim to be sure we have at least one in the office that supports the diagnosis. I encourage patients to have some ambulatory readings before diagnosis – easier with some patients than others.
I don't use 7 days am and pm and am not sure how, for example, continuous ambulatory BP monitoring fits in a risk reduction campaign – they did not do that in the VA studies to my knowledge. It seems like one of those places where we have to wonder how much better than better can we get (like thinpreps)? I do counsel on technique, primarily sitting with feet on the floor and resting for at least a few minutes before taking (not sure how many will sit for 5 minutes each time). And while I think it is good to be able to monitor at home, I think we should be careful to use monitoring to support action (either lifestyle or medication changes) rather than monitoring to support worry (twice daily every day).
I don't recommend certain types of monitors because I don't know that I can keep current with model changes – I've usually referred patients who want to buy one to have a discussion with their pharmacist. Consumer reports had a recent review though, so now I can point patients to that.
Marc
Hi Mark,
Don't be sorry, thanks for reading and following along. Actually, continuous ambulatory BP and home BP are not the same thing. The AHA, in its May, 2008 position paper, proposed periodic 7 day readings (q-quarter). These are actually more predictive of morbidity/mortality than office readings. 20% of office readings are falsely elevated, and result in unnecessary treatment. 10% (and maybe more due to the 'dental flossing effect') are falsely normal, resulting in not enough treatment.
What we found in going through the cycle with the patient was an interesting phenomenon, which was the imposition of the doctor's beliefs and values over the patient's, resulting paradoxically in less adherence and confidence in the treatment plan.
The comment about supporting worry – I don't think the studies on patients doing self-monitoring show that. Consider the idea that when we tell patients, "the determination of your blood pressure happens in my office, and not in your environment" may actually support worry, and in one BMJ-published study, patients actually felt less confident in a blood pressure taken by their doctor than one they did themselves.
In addition, I have seen physicians recently counsel patient to do home monitoring without any parameters, and at the same time, I talk to other patients who interpret that to mean "check it whenever, wherever." What we can do as physicians is be more clear by saying, "Check it just twice a day, don't take your cuff to work, just once in the morning, once in the evening, for 7 days, that's it."
What I'm interested in looking at is whether involving the patients more rather than less will produce better outcomes, and deploying the technology we have to do so, now that it's here. The Green, et. al study points to that possibility. It seems we can't do worse – I think we have to look at the results of our actions so far as a health system – only 1 out of 3 patients with blood pressure are under control, and most of these patients are insured and receiving medical care,
Ted
The AHA position statement on HBPM is very interesting. The prospective cohort studies which show a stronger association for HBPM vs office monitoring fit with what we both commonly experience in primary care – the white coat syndrome. I didn't go through and read each of those five prospective studies, but the AHA paper does not describe any of them as randomized. We should at least speculate whether any bias could confound the findings. In contrast, studies we have relied on for confirmation of the benefit of treating hypertension (most recently ALLHAT) used office testing to assess response to treatment – we shouldn't completely throw out office readings. The cohort prospective monitoring studies certainly suggest treatment benefit may be even more dramatic if HBPM were used. Will future randomized studies employ this?
The model you are suggesting would place the office BP measurement in the hypothesis generating realm – it would trigger confirmation in the home setting for those that enter the path of hypertension diagnosis and management through the office (those patients easily within my sphere of influence). I agree with this. The AHA call to action for reimbursement for home monitors is on target. Not all insurers agree with this now, however.
Given the high prevalence of undiagnosed hypertension and the apparent cost effectiveness of diagnosis and treatment, why shouldn't we adopt a strategy of issuing a loaner home cuff to all people in a target population (maybe 30+ adults) for an annual home BP study week? As a population strategy, who should be doing this? Employers could probably do more with this than the current trend of employer sponsored weight loss programs.
The imposition of beliefs and values comment: if I present high BP as a finding, discuss risks of untreated HTN, give the patient an opportunity to assess at home to support the diagnosis, then discuss lifestyle and medication options for management, am I still imposing 🙂 ? Can you suggest how we can better avoid imposing?
The worry comment I made is for the twice a day every day patients, and stems from my (imposed on patients at times) belief that you should have an idea what you will do with the test results before you perform the test. I think you understood differently for that comment to mean that I don't value the home readings. That is not the case. My routine follow up for an abnormal reading in the office is for the patient to monitor outside the office and report back (we call them) in 2-4 weeks. However, I do understand for some people daily HBPM is part of their motivation for daily adherence, so I'll retract the worry comment.
I could probably do better with specific guidance on ambulatory monitoring. This looks like a good place for a handout. Any specific reference handouts you suggest? Save me time abstracting the useful ideas from the AHA article.
Hi Mark,
Good ideas all around – don't you think they make a good platform for a pilot program funded by an innovative Foundation? 🙂
I think you're right that a change in practice would benefit from good patient education, and good workflow. We're really on the ground floor because we've been wedded to the office-version of health care for so long, and as you say, there aren't a lot of financial incentives driving a change to a more patient-centered approach. I'm interested in working on all of these, not just some of them, because they have not been figured out.
On the imposing question – If I wasn't 2,300 miles away, I'd be happy to shadow you in person. Better than me telling you how your patients feel (and what do I know), why not ask your patients after the visit?
You could ask how confident are they in managing their condition. What about your discussion empowers them, and is there anything more you could do? Are the answers different for those that are controlled or those that aren't? Feel free to repost their answers here (if it's appropriate).
Worry comment is duly retracted. This is a journey, not a destination, and I appreciate that a medium like this allows us to learn from each other about how to improve the care of patients, with the patients present. That part is pretty awesome I must say,
Ted